|
|
Lymphoedema
Lymphoedema is a condition caused by dysfunction or damage to the lymphatic system. The lymphatic system is responsible for removing and filtering waste products, fluid and proteins from the body’s tissues. If the system is unable to cope, the tissues accumulate fluid and proteins which can cause the area to swell, the skin can harden and change and the condition can become severe if not properly managed.
Lymphoedema has two main causes:
Primary lymphoedema is caused by insufficient sized, shaped or numbers of lymphatic vessels or nodes. This is a congenital condition, although symptoms might not develop until the patient is in their teens or young adulthood.
Secondary lymphedema is caused by damage or trauma to the lymphatic system. In the Western World this is usually from surgery, lymph node removal or radiation for cancer. Anyone who has any or all of these procedures is at risk of developing lymphoedema at any stage in the future.
Signs of lymphoedema
Lymphoedema has two main causes:
Primary lymphoedema is caused by insufficient sized, shaped or numbers of lymphatic vessels or nodes. This is a congenital condition, although symptoms might not develop until the patient is in their teens or young adulthood.
Secondary lymphedema is caused by damage or trauma to the lymphatic system. In the Western World this is usually from surgery, lymph node removal or radiation for cancer. Anyone who has any or all of these procedures is at risk of developing lymphoedema at any stage in the future.
Signs of lymphoedema
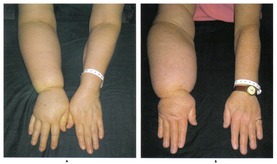
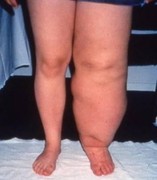
- Gradual swelling of the affected limb. It’s rare for more than 2 limbs to be affected.
- The area may feel heavy or taut
- Skin may pit initially
- Skin folds at the joints become deeper and more pronounced.
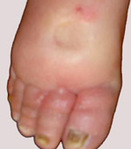
- A positive “Stemmer’s Sign” test – when the skin on the second toe or finger of the affected limb is pinched, it cannot be raised and feels taut and hard.
- As the condition develops, the skin and tissues become hard and fibrotic.
Diagnosis
Lymphoedema is mostly diagnosed using palpation and observation, combined with a medical history. There are some tests that can be done using modern medical imaging, including lymph scintigraphy, if confirmation is required.
Treatment
This condition cannot be treated with diet or medication, nor is there a cure for lymphoedema. It is a chronic condition that requires ongoing management.
The first-line therapy is Combined Decongestive Therapy (CDT), consisting of Manual Lymphatic Drainage, exercise, skincare and compression of the effected area.
There are two stages of treatment. The first is the Reduction Phase, which involves 3 weeks of daily treatments and bandaging to reduce the size of the limb and bring side effects under control.
Phase 2 is the Maintenance Phase, whereby the reduction is maintained with ongoing CDT.
Lymphoedema is mostly diagnosed using palpation and observation, combined with a medical history. There are some tests that can be done using modern medical imaging, including lymph scintigraphy, if confirmation is required.
Treatment
This condition cannot be treated with diet or medication, nor is there a cure for lymphoedema. It is a chronic condition that requires ongoing management.
The first-line therapy is Combined Decongestive Therapy (CDT), consisting of Manual Lymphatic Drainage, exercise, skincare and compression of the effected area.
- Manual Lymphatic Drainage (MLD)
- A gentle, subtle massage technique that works to stimulate the initial lymphatic vessels in the first layers of skin to open and drain towards functioning lymph nodes. Although many therapists are trained in MLD, it’s important to seek out a therapist trained in the advanced MLD techniques of lymphoedema management, as they have the additional knowledge to understand the adjustments needed to work around a lymphatic system that isn’t functioning correctly.
- Exercise
- Gentle, progessive and rhythmic exercise is recommended to improve lymphatic flow.
- Compression
- In the reduction phase of treatment, compression will usually take the form of multi-layer bandaging or adjustable wraps. Once reduced, the patient will be fitted for a compression garment. Amanda will work with you to prescribe the best type of garment for your needs.
- It's essential to wear proper compression garments when flying or sitting for long periods of time, even for those who are at risk of, but haven't developed lymphoedema.
- Lymphtaping
- Uses soft, flexible fabric tape called kinesiotape to assist lymphatic drainage following treatment. The tape can be worn for a week, is water-proof and hypo-allergenic. It's also useful to use in areas that are difficult to compress, such as in cases of head and neck oedema, breast oedema and seromas and abdominal areas.
- Low Lever Laser Therapy (LLLT)
- A painless, non-invasive treatment tool that therapists as an additional tool alongside CDT to reduce hardened fibrotic tissue and scar tissue, improve recovery time, reduce swelling and inflammation and improve mobility and skin condition. The infrared light works at a low frequency to penetrate into the tissues below the skin. Treatments are usually 15-20mins long and should be carried out at least 3 times a week for 3 weeks.
- Intermittent Pneumatic Compression (IPC) Pump
- IPC is another tool to be used alongside CDT. The patient wears an inflatable sleeve on the effected limb which then runs on sequence inflating and deflating to mimic MLD.
- Amanda is currently trialling a pump in clinic. One of the benefits of the pump means that clients can increase the frequency of treatments at a lower cost.
- Clients can also buy their own pump and use daily at home for ongoing long term management. Amanda is happy to guide you in your purchase.
There are two stages of treatment. The first is the Reduction Phase, which involves 3 weeks of daily treatments and bandaging to reduce the size of the limb and bring side effects under control.
Phase 2 is the Maintenance Phase, whereby the reduction is maintained with ongoing CDT.